2022 Impact Report
Research:
Saving and improving lives
Today’s research empowers tomorrow’s breakthroughs
Research improves the quality of health care, treatments, interactions and experiences for patients and their families.
Research projects funded by Calgary Health Foundation have bold visions to reshape care and address gaps in the health care system.
While these research projects are in the early stages and focused on Calgary, each one has already garnered broader interest due to their progressive and innovative topics.
Cohort study for preterm birth
Types of research:
Investigating the mechanisms of health and disease
Applied research to advance care
$5M
IN PARTNERSHIP WITH
ALBERTA CHILDRENS HOSPITAL
Project completion estimate: 2024 (five years)
Of the more than 17,250 babies born in Calgary each year, about 1,550 are born preterm. Over 1,200 of those preterm infants require specialized care within a neonatal intensive care unit (NICU). In addition to the strain on families, the estimated annual health care costs associated with caring for preterm infants in Canada is $587 million.
This research focuses on the prediction, prevention and intervention of preterm birth. A team of scientists and care providers based out of the University of Calgary is inviting 4,000 expectant mothers from Calgary and southern Alberta to participate in research that will take place throughout their pregnancy and up to one year after they have delivered their babies. Fathers and partners are also encouraged to take part.
In the first phase of the initiative, which is now underway, scientists are working in the lab to develop a blood test for rapid diagnosis. This research asks questions about if, and gestationally when, maternal biomarkers can predict preterm birth.
The teams will also use the power of advanced machine learning to generate personalized risk scores for pregnant women, enabling health care professionals to anticipate preterm births and provide care strategies tailored for individual families.
Projects supported through this investment
Prediction
- Integrating maternal biomarkers for predicting preterm birth
- Early discoveries from this research:
- Repeated sampling (i.e. change in biomarker expression) during the second and third trimester is a promising avenue for biomarker discovery.
- Preliminary analysis using machine learning has identified novel biomarkers and highlighted potential new pathways involved in the mechanism of preterm birth.
- Early discoveries from this research:
- Using machine learning to predict spontaneous preterm birth
- Biomarkers of imminent preterm birth in high-risk women (P3 High Risk Cohort)
Prevention
- Income assistance for low-income women (currently under ethics review for approval)
- Remote peer-counsellor-delivered behavioral activation and peer-support for antenatal depression on gestational age at delivery: a single-blind, randomized control trial
Intervention
- The role of inflammation in brain injury and development of preterm infants
- Optimizing family health following preterm birth
- Digital parenting interventions for fathers
- Do children born preterm play ‘catch-up’?
Hypoxic-ischemic encephalopathy
Types of research:
Applied clinical research advancing care
$894K
TOTAL INVESTMENT
Estimated completion: ongoing (multi-year)
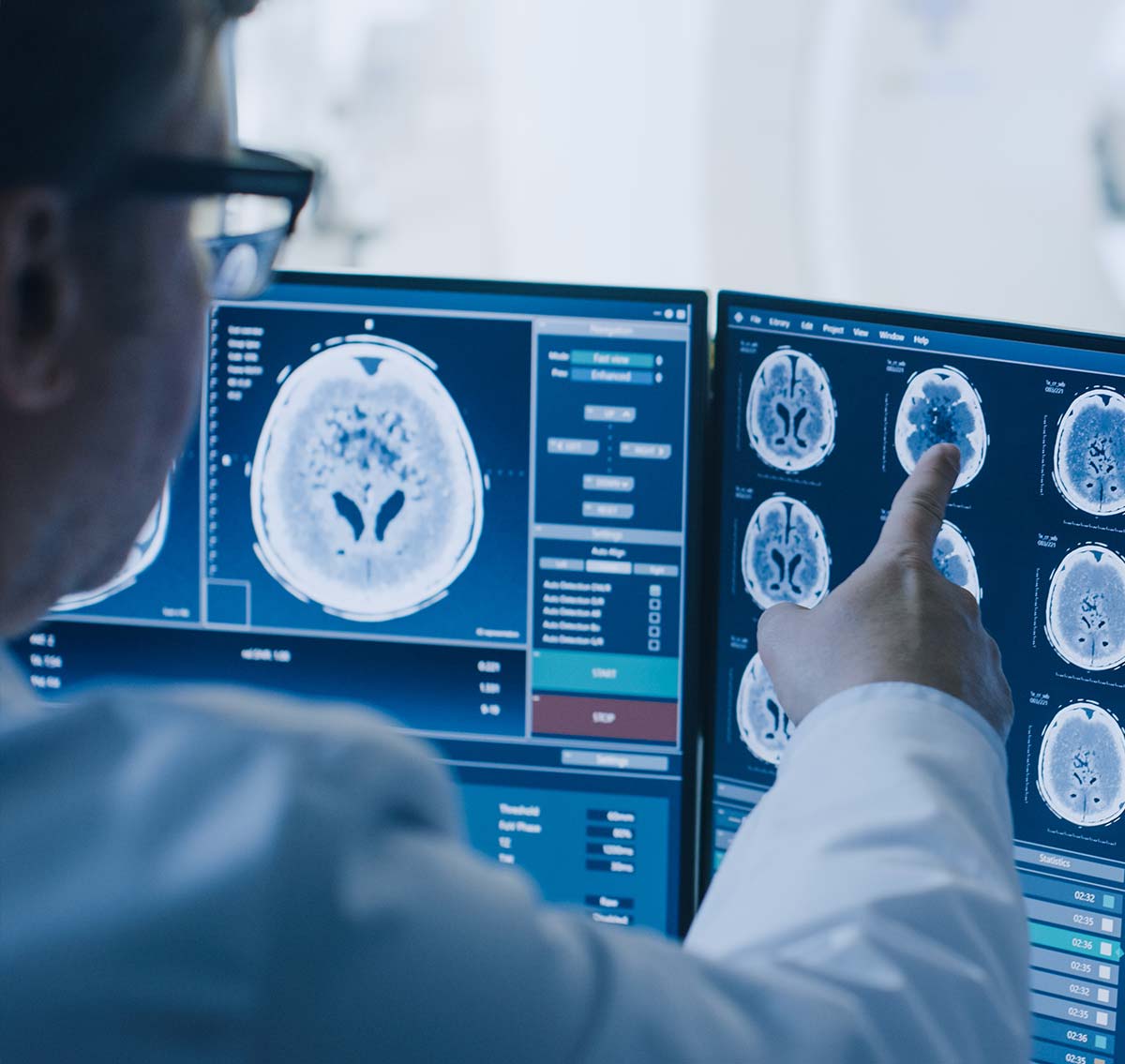
Hypoxic-ischemic encephalopathy (HIE) can result from limitation of oxygen and blood flow to the brain around the time of birth. HIE can cause brain injury and result in cerebral palsy and other cognitive and developmental impairments. Neonatal asphyxia is one of the most devastating potential outcomes of pregnancy; with long-term impacts on the infants, families, and health care systems. A single HIE case can cost in excess of $1.5 million over a lifetime of care.
This research project has established the largest database of its kind globally, using data from across the province to understand current HIE diagnosis, monitoring, management, and follow up with the goal of establishing best-in-class standardized care protocols.
Through education and standardization, early identification of HIE and deployment of time-sensitive cooling protocols can prevent detrimental effects for many newborns.
EMBER: Stigma in the emergency room
Types of research:
Health services and policy research

$898K
TOTAL
INVESTMENT
Project completion estimate: 2026 (five years)
Annually, one in five Canadians face challenges pertaining to their mental health, making it the leading cause of disability in Canada.
The prejudice and discrimination that can exist around mental illnesses is a barrier for many in receiving vital support at critical times. The access point for critical, and sometimes life-saving, support of urgent mental health concerns often originates in the hospital’s emergency room. This very first interaction can drastically influence a patient’s journey and outcomes.
The Exploring Mental Health Barriers in the Emergency Room (EMBER) research aims to explore mental illness-related stigma experienced by patients and families in hospital emergency departments.
This study will also examine staff members’ experience of mental illness stigma and the impact this can have on their ability to provide care, as well as their own willingness to seek care for themselves when needed. In partnership with Alberta Health Services, the research team will also work collaboratively with the policy services team to examine and improve policies related to access and the provision of mental health services.
Early findings from stakeholder consultation in this research:
- Identified several manifestations of stigma that cause harm to patients, and confirmed need to advocate for structural changes.
- Emphasized need for more education and training for providers in mental health and substance use to build confidence and improve care.
- Highlighted interconnection between mental heath and occupational stress of frontline health teams and quality of patient care, in what can be very challenging and demanding environments.
- Reiterated importance of physical space redesign to improve care for mental health patients and families.
- Confirmed the need to build trauma and resiliency focused cultures of care and physical environments.
- Acknowledged value of specialized peer support for mental health and substance use that can be integrated into healthcare teams, to provide advocacy and support to patients and families and better connection to community services.
Improving methamphetamine toxicity treatment
Types of research:
Applied research to advance care
Advancing health services and policy
$159K
TOTAL INVESTMENT
Estimated completion: 2023 (two years)

This research focuses on the intersection of healthy behaviour, access to health care and the right to live at-risk while using substances, with the vision to inform and improve the care of a historically marginalized and vulnerable population.
The goal is to create standard treatment protocols for patients who present with methamphetamine intoxication. These individuals may enter their care journey at a hospital or via a community organization.
Standardizing treatment protocols will result in a focus on wellness for care providers and better outcomes for patients.
Early on, this research garnered national attention as many hospitals face similar circumstances and need to provide better support for both the patient and care provider in cases involving methamphetamine toxicity.
Precise-MH: Mental health & addictions data
Types of research:
Advancing health services and policy research
Population and public health research
$892K
TOTAL
INVESTMENT
Estimated completion: 2025 (four years)
There are many unique and complex factors contributing to the relationship between Alberta Health Services addictions and mental health team, homeless shelters and police services.
The goal of the PRECISE-MH study is to improve understanding of the relationships between these three entities in Calgary and create stronger links in sharing data and analytics that will ultimately result in a more integrated approach to support services for vulnerable individuals.
Preliminary data indicates that there are approximately 800,000 individuals age 18 to 65 who are identified as having a substance use and/or mental health issue in the province of Alberta as of the study entry date of April 1, 2018.
Quick facts:
Serious mental illness is 10x more common in individuals experiencing homelessness.
Substance use and mental health are over-represented among people in contact with police.
Access to mental health services among people experiencing homelessness is limited due to stigma and poor integration of services.

